Reading Time: 6 Min
Since every mother wants her baby to have the best nutrients in the world and nothing compares to breast milk, breastfeeding after breast surgery is a major concern for most women who want to undergo this procedure.
Of course, breast surgery affects the size and shape of breasts but will it affect the milk supply? We will find out soon.
In this article, we will walk you through breastfeeding after breast surgery to answer all your questions and concerns so you can make an informed decision.
To understand if your breast surgery can affect breast milk production and release, you should first quickly review how breast milk production works.
How does breast milk production work?
The truth is all postpartum women can supply some droplets of colostrum (first milk) regardless of their previous breast surgery, but each individual is different. The colostrum is believed to be the most nutritionally dense substance for the baby.
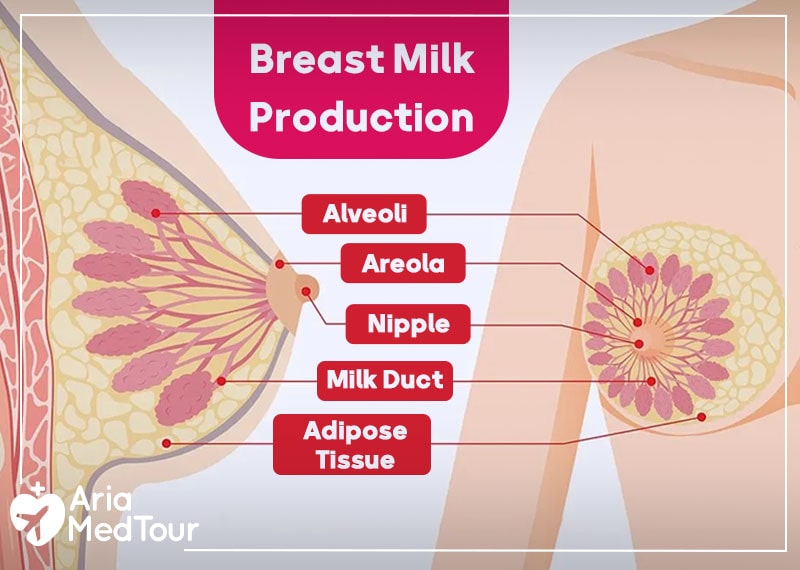
Milk is produced from mammary glands that consist of alveoli and ducts in which milk is produced and stored within the alveoli and travels through the ducts to the nipple.
Milk production is a complex process that depends on many physiological and psychological factors such as the anatomy of the breast, existing health conditions, essential nutrients, emotional state, and the latching ability of the baby.
How does breast surgery affect breastfeeding?
Breast surgery is performed for different reasons, mainly cosmetic or diagnostic surgery.
In either case, you should discuss your pregnancy and breastfeeding plans with your surgeon so the doctor can inform you how the procedure will impact your plans which depends on the following factors:
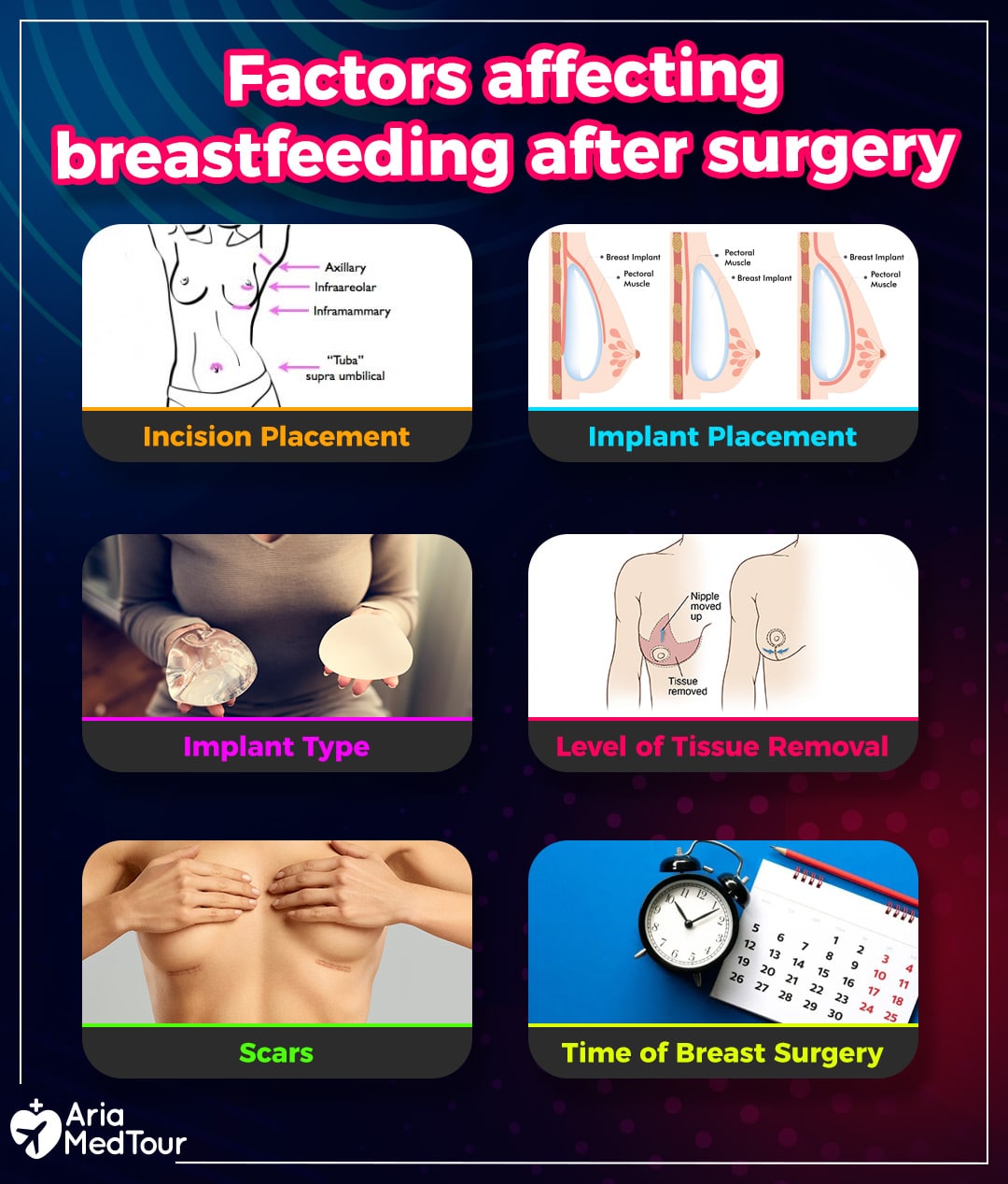
● The placement of the incision
If the incision is done in the underarm, breast crease, or belly button, the chance of damage to milk ducts or nerves is very small. In the case of incision at the edge of the areola, it is performed at the surface level while the nerves and milk ducts run from below toward the nipple, so the chance of cutting them is still low. Of course, the surgeon’s expertise will be critical in staying on the periphery of the areola and preventing any damage to the underlying structure.
● The placement of breast implants
Breast implant placement can be over or under the muscle of the chest wall in which the former (Subglandular) might put pressure on the glandular tissue that affects milk supply. It can also cause engorgement issues in which the breast becomes tense and full. In contrast, the latter (Submuscular) have almost no interference with milk production and release.
● The type of implants
Silicone implants are non-absorbable by the body, so they shouldn’t be a problem. According to a 2001 report by the American Academy of Pediatrics (AAP), there was insufficient evidence to justify classifying silicone implants as a contraindication to breastfeeding.
The body will absorb saline-filled implants in case of a rupture which is a safe solution, so there is almost zero concern.
● The level of tissue removal
Breast reduction is the most concerning when it comes to milk production if the areola, nipple, and the tissue beneath them are removed during surgery. The reality is that your goal is to reduce your breast size, so some tissue (mainly fat) will be removed, but some milk ducts and nerves might be cut, and the nipple might be moved. The good news is that glandular tissue will grow again during lactation, improving milk production over time. In addition, new surgical techniques aim to protect mammary glands and nerves as much as possible.
The nipple surgery has minimal tissue removal from the skin that does not touch mammary glands.
In breast lift or mastopexy procedure, the skin is the focus of the surgery since it is not strong enough to hold the underlying tissue. So, the excess skin will be removed, and not much underlying tissue will be touched.
In breast cancer surgery, only the abnormal tissue and a small amount of surrounding healthy tissue will be removed, so the possibility of significant damage to mammary glands is very low.
In the breast augmentation procedure, there is almost no tissue removal since the goal is to enhance the size by adding an implant.
● The scar formation
Another critical factor is the gradual scar formation that occurs in the weeks post-procedure. Although rare, it can clog the ducts and block the milk from traveling to the nipple. However, it depends partly on your ability to heal and your commitment to follow the post-operative instructions given by your doctor. The other part is the expertise of your doctor in fine surgical sutures that do not form large scars and remain invisible.
If you choose to have nipple jewelry, consider the timing since recent piercing scars may not heal for the time of breastfeeding. Removing nipple jewelry in the second trimester of pregnancy is also recommended, and keeping it off during breastfeeding since there is a high risk of infant choking.
● The time of breast surgery
According to La Leche League, if the surgery has occurred more than five years before pregnancy, the milk production will be significantly better because ducts or nerves that were severed during surgery will grow back and form new pathways to regain milk production functionality.
How to increase milk supply after breast surgery?
Lactation help is available to increase milk supply so your baby can have all the necessary nutrients.
The optimal solution is your baby that latches frequently and effectively in the first two weeks since the more milk is removed from the storage, the more will be produced, and your body will determine the course of milk production from thereon.
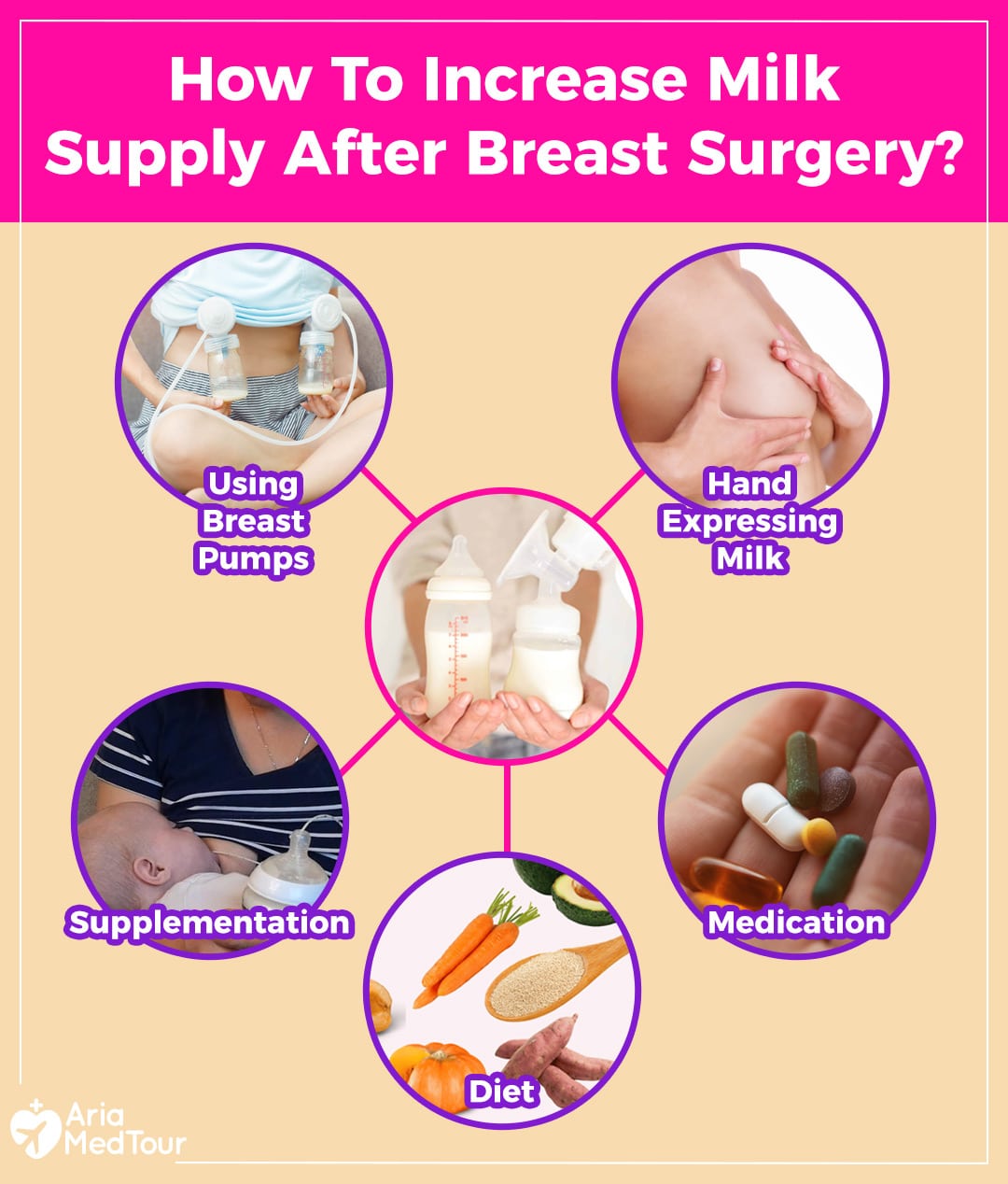
A lactation consultant can guide you toward the right actions, but you can do simple things to encourage milk production:
1. Express your milk by hand
Hand expressing colostrum every 2 to 3 hours in the first few days is critical that initiates the course of milk production in the coming months. Your baby’s weight check determines if enough milk is supplied.
2. Use breast pumps
A double-electric breast pump is a great option to increase milk production while managing engorgement. Do it after each nursing or more than eight times a day for 5-10 minutes, even if your baby is not latching at the breast.
3. Use supplementation
If you couldn’t exclusively breastfeed your baby, supplementation with pasteurized donor milk or formula is always available that can be used with a feeding tube or a commercial product. They consist of a container that holds the supplement and a tube that runs to the nipple allowing the baby to latch at them both.
4. Use herbal galactagogues
Herbal supplements that are categorized as galactagogues can increase milk supply. However, discuss your choice with your physician first to prevent side effects. Some foods can have the same impact, so maybe a dietitian can help you with a diet plan to increase milk production.
5. Take medications cautiously
Some medications can induce lactation while others inhibit lactation; therefore, the latter should be avoided as much as possible.
Conclusion
In most cases, you can breastfeed after breast surgery since surgical techniques and technologies have evolved significantly to prevent damage to mammary glands and nerves.
After all, 300,000 breast surgeries are performed annually in the US alone, so it shouldn’t cause breastfeeding problems; otherwise, young women wouldn’t accept such a risk.
In the end, breastfeeding is an intimate skin-on-skin relationship between you and your baby so use the breastfeeding tips offered in this article to nourish your infant with every drop of your precious breast milk after breast surgery.
Breast Augmentation in Iran
Surgery + Hotel + Visa
Transfer + Interpreter
Related Articles
Feel free to express your opinions or ask your questions regarding the article






My baby has been fed for 10 months, is the time too short?
You won’t be able to breastfeed until 72 hours after surgery. so you can express your milk and store it in the refrigerator for the first 72 hours post-surgery.
I had a breast reduction a few months ago and now that my baby is here, I’ve noticed my milk supply dropped after surgery. I’m worried this might be permanent. Is breastfeeding after breast reduction always this challenging, or does the supply improve over time?
Hi Emily! It’s completely understandable to feel concerned. A reduced milk supply after surgery can happen, especially when glandular tissue or milk ducts were affected during the procedure. However, breastfeeding after breast reduction is still possible for many mothers, and supply often improves with frequent nursing, pumping, and proper lactation support. We recommend consulting a lactation specialist to create a personalized plan and monitor your baby’s intake.